
Executive Summary
The treatment of pneumonia patients is weighed heavily in Saint Luke’s University Health Network (SLUHN) national pay for value programs. Performance around mortality and readmissions can result up to a 3% penalty for hospitals across the nation and performance is publicly reported through the Centers for Medicare and Medicaid Services (CMS). To improve the overall care of SLUHN pneumonia patients, the Network Pneumonia Performance Improvement team conducted multiple chart reviews to identify trends demonstrating opportunities to improve care. The team identified the need to standardize treatment for patients with a diagnosis of pneumonia. In review of the literature, the Infectious Disease Society of America (IDSA) discussed the need to revise their current recommended treatment guidelines for patients with health care associated pneumonia (HCAP) based on new evidence findings.
In reviewing SLUHN performance for pneumonia patients utilizing All Patient Refined Diagnosis Related Group (APR DRG 139) risk adjusted classification, all payers, we identified that our performance was far from desired in our quality fiscal year (FY) outcome measures. SLUHN’s network performance in length of stay, mortality, and readmission performance was either at the 50th percentile ranking or less compared to other like size hospitals participating in the CMS Hospital Readmission Reduction Program.
A network pneumonia treatment guideline was created to standardize care for pneumonia patients. An order set was created that would mirror the recommended pneumonia treatment guidelines that were established. Antibiotic choices were reviewed by pharmacy and infectious disease physicians to ensure that the pneumonia guidelines would be in line with our antimicrobial stewardship as well as meet the sepsis protocol recommendations within the Epic order set. Additional interventions were also taken to improve the overall outcomes of our pneumonia patient population.
The improved outcomes of the pneumonia guidelines were measured by readmission and mortality performance for those patients who had the pneumonia order sets used during their inpatient stay. In comparing FY17 to FY18, there was a reduction in the mortality index by 35%, making it statistically significant, for those patients that had the pneumonia order set used compared to those that did not. The readmission index was reduced by 26%, statistically significant, for those patients that had the pneumonia order set used in the acute care population versus those that did not. In comparing those patients who had the order set utilized versus those that did not, there was a cost savings of $6,370,561. The performance across FY19 has also maintained and remained statistically significant in mortality and length of stay outcomes.
Define the Clinical Problem and Pre-Implementation Performance
In 2008, CMS established a program known as Value Based Purchasing (VBP) that ties patient outcomes and performance with payment. The goal of this program was to improve quality of care, provide patient centered care, and increase accountability of organizations. Multiple measures were established in this program, some of what included:
- 30-d risk standardized readmissions for pneumonia
- 30-d risk standardized mortality measure for pneumonia
On a quarterly basis, performance is reported on a hospital compare website to improve transparency in health care and the community in which we provide our care. Additionally, CMS develops benchmarks for performance in these measures based on previous years’ national benchmarks. Based on each hospital’s performance, 2% of payment is withheld by CMS and redistributed to hospitals by awarding good performers and penalizing poor performers. This 2% equates to approximately 1.9 billion dollars of re-distributed money nationally for healthcare organizations.
Other programs that also impact our organization regarding the care we provide to our pneumonia patients are:
- The Hospital Readmission Reduction Program (HRRP) is a payment program also established by CMS that penalizes poor performing hospitals up to 3% of their payment based on an excess in readmissions. The goal of this program is to improve healthcare for all consumers.
- Highmark Incentive Program- 90-day episode of cost and spending measure for the pneumonia population and 7-day discharge follow up from the hospital.
In FY17, our observed over expected (index) performance in the all-payer pneumonia readmission population using risk adjusted APR DRG: 139 classifications:
- Length of Stay (LOS): .96 (50th percentile)
- Readmissions: .91 (Below 50th percentile)
- Mortality: .68 (45th percentile)
In 2016, multiple chart reviews were conducted in response to our poor performance in readmissions, LOS, and mortality to identify a trend of potential opportunity. The multidisciplinary Network Pneumonia Performance Improvement (PI) team identified through these chart reviews that the most common theme of opportunity was the lack of standardization for treatment of pneumonia (Figure 1).
A literature review was conducted and found that according to recommended IDSA guidelines published in 2005, our organization had an opportunity to define a treatment guideline for pneumonia. Furthermore, other literature and health systems supported the implementation of a pneumonia pathway which demonstrated positive results in reducing readmissions and mortality over 20%. Based on our findings in the literature review, the overall objective was to determine if the utilization of high and low risk clinical pneumonia guidelines would, using an order set, (a) reduce 30-day readmissions, and (b) reduce mortality by 20% in the acute care pneumonia population.
Design and Implementation Model Practices and Governance
A fishbone diagram was developed to define root causes of inconsistencies in pneumonia care practices and to define areas of focus from a governance perspective.
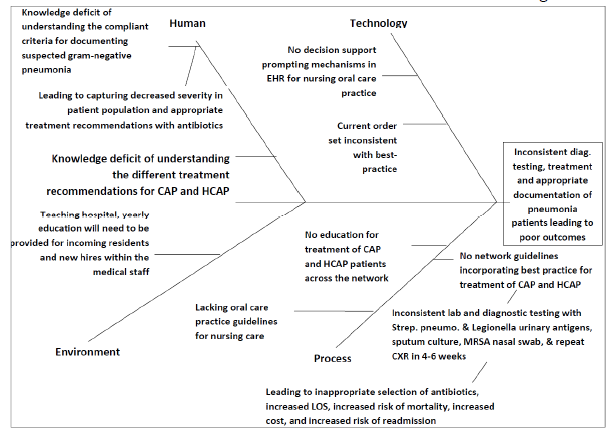
Source: St. Luke’s University Health Network
This project is an organizational priority to improve overall compliance in the treatment and best practice of those pneumonia patients entering the St. Luke’s University Health Network. Improving overall pneumonia readmissions and mortality publicly reported outcomes also were made a priority. Stakeholder buy-in was obtained through administrative and clinical specialty support over the Network Pneumonia PI committee. Infectious disease and pulmonary providers were also consulted regularly.
The following best practice interventions were put into place to address pneumonia performance:
- In review of more recent literature, anticipated new guidelines were created for the network. As per prior recommendations, all patients coming from or exposed to the health care environment were placed on broad-spectrum antibiotics. However, newer recommendations were to review those patients who had higher risk for exposure to multi-drug resistant (MDR) organisms, and if they did not meet criteria, would be treated with CAP (low risk) antibiotics. This was not previously done. Guidelines were created with a pneumonia pathway and an order set that mirrored the flow chart and pneumonia guidelines created.
- Panels were built in the ED order sets that complied with sepsis guidelines but also complemented the IDSA recommended guidelines for treatment of pneumonia.
- A pneumonia zone tool from the Agency for Health Research and Quality (AHRQ) was modified for patients to improve transition of care and recognize signs of early deterioration after leaving the hospital. The zone tool was integrated into education templates in Epic to ensure that the information would be pulled into discharge documents known as the After Visit Summary (AVS) at discharge. (Figure 1). (https://www.ahrq.gov/tools/index.html)
- An oral care bundle was created and piloted on an inpatient unit with the highest hospital acquired pneumonia events.
- Order set utilization was only reported by Epic within a 90-day period due to the large amount that could be accommodated within Epic. As of March of 2019, a Tableau report was created to reflect the count of order set utilization. This was integral in determining the quality outcomes the revised order set would have on the pneumonia population.
- A learning management system was used by our network’s internal instructional design team to create an e-learning that was implemented at the beginning of this project. This e-learning served to educate providers on the process and order set utilization within Epic. Additionally, this e-learning became part of the orientation program for newly hired boarding practitioners as a way to capture every provider who treats pneumonia in the network.
Figure 1: Pneumonia Zone Tool
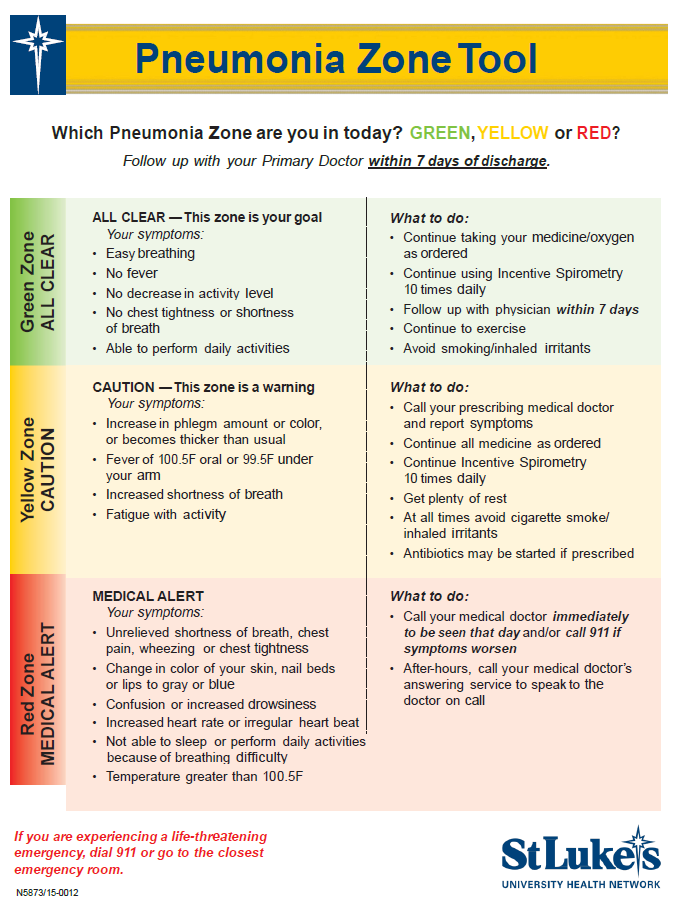
Source: St. Luke’s University Health Network
See graph below to annotate important points of change while implementing these initiatives (the newly revised order set was used to demonstrate the standardization in provider practice):
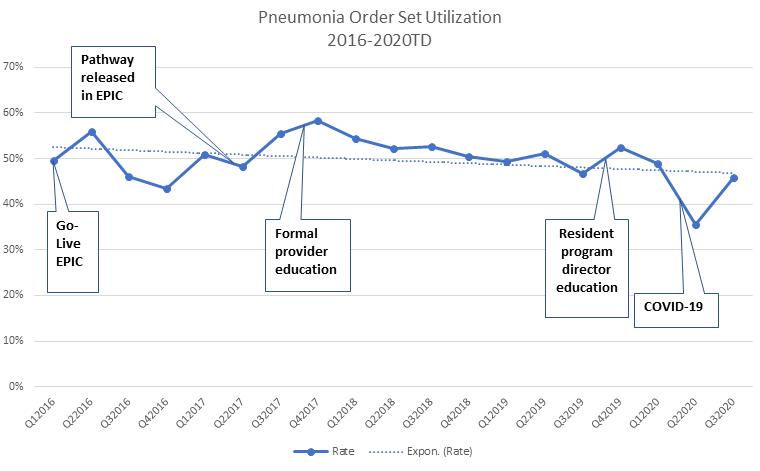
Source: St. Luke’s University Health Network
Clinical Transformation enabled through Information and Technology
Initiatives implemented and integrated into the nursing and clinician’s workflow was building the pneumonia zone tool recognized by the Agency for Healthcare Resources and Quality (AHRQ) (https://www.ahrq.gov/tools/index.html) into the electronic health record and was included in the after-visit summary at discharge. Additionally, nursing had the pneumonia zone tool integrated into their care plan documentation in the electronic health record. The pneumonia zone tool is a standardized post-diagnosis and preventative care pathway for those patients diagnosed with pneumonia. It was created to better assist patients in better self-management of their symptoms, as well as assist with reducing a patient’s chance of readmission. This tool also allows providers to assist in patient education by providing a visual, easy, step-by-step guideline that explains what to look for as patients progress through their healing process.
A network oral care bundle was implemented by modifying the current documentation flowsheet rows and customizing them to match our current supplies and recommended practice. A task worklist was created for nursing staff whose patients were ordered routine oral care. Compliance of these initiatives was monitored by leadership by performing audits of EMR documentation.
An EHR order set for the treatment of low and high-risk pneumonia was created with the goal to be all-inclusive and evidence-based. Any patient that is admitted with the clinical signs and symptoms of pneumonia (cough, sputum production, fever, chills and or trouble breathing) will undergo initial workup to rule out or include pneumonia as an admitting diagnosis. Patients will undergo lab work and cultures (including CBC with diff, Procalcitonin, COVID-19, Blood cultures) as well as a chest X-ray. If evidence demonstrates that a patient may have pneumonia, the patient is then started on the pneumonia pathway.
Implementation and Standardization of Pneumonia Treatment Guidelines
The team created a multi-drug resistant (MDR) risk stratification tool for antibiotic selection within the EMR order set with the intent of guiding clinicians on patient treatment. Upon initiation of the order set, there is a risk stratification tool for those patients who are at high or low risk for MDR pneumonia. If a patient has one or less risk factors, the provider will then follow the pathway for the low risk MDR pathway. If the patient has two or more MDR risk factors, the provider will then place the patient on the high-risk pathway. The EMR order set directs the clinician through the order set based on those risks. The antibiotic choice is dependent on the MDR risk factors, allergies, and whether the patient is septic or not. The patient will then be initiated on the correct antibiotic choice within no more than four hours of admission.
The team implemented the use of preselected orders within the order set. These preselected orders can be unchecked if deemed clinically irrelevant; however, these are orders that are aligned with the pneumonia clinical guidelines from the IDSA as well as areas of prior noted poor compliance, within the network. In order to improve overall compliance and outcomes and added descriptors within the orders, a hyperlink was added to the order-set that if clicked, would take the clinician to the network clinical practice treatment guidelines for pneumonia and detailed guidelines to simplify the process of following the treatment guideline for pneumonia. The team created fully detailed, evidence-based and antibiogram-approved antibiotic choices, which were embedded in the order-set for selections to be made based on the MDR risk stratification tool. Orders were built to cascade open as the provider advances through the workflow in order to not overwhelm the ordering provider with unnecessary selections.
Once the order set and new workflow was created and ready to be implemented, all treating providers needed to be educated by the IT training and operational teams. Provider education was implemented through My-E-learning (MEL), network education platform, for those pertinent groups and those being on boarded into those groups. The My-E-learning provider education was mandated to be completed by all providers within the network who diagnose and treat pneumonia. It was also provided to all new onboarding providers within the network. Education was provided through E-learning and then later reinforced by a small, specialized group, consisting of a clinician, a quality manager, a pharmacist, and a documentation specialist. A “road show” was started, and all campuses were visited by the group. Presentations were completed at all campuses within the network. A presentation was provided to our residency service on multiple occasions. Posters were provided for offices and guidelines have been permanently embedded into the order set as a hyperlink, which can be updated as guidelines change.
Improving Adherence to the Standard of Care
Our education platform was used at the beginning of this project to educate providers on the process. We added the E-learning be a part of the orientation program of learning for on boarding practitioners to capture every provider who treats pneumonia in the network.
Additionally, routine feedback was sought from providers who did not utilize the order set. This feedback was used to improve the workflow of the order set and encourage its adoption into their practice. Some examples of this rapid test in change are as follows:
- Urine for legionella and strep pneumoniae were pre-checked as this was per the recommendation of the IDSA guidelines. Our collected data demonstrates that the majority of these studies were negative, therefore, resulting in increased cost and low yield. After review, this was then unchecked with additional verbiage added to the order. For example, recommendations to order the legionella urine test in only those patients who are critically ill, immunocompromised or during warm, humid months.
- Obtaining 2 sets of blood cultures have been recommended prior to antibiotic therapy in order to better diagnose and treat certain organisms.
- Later in the year, a Procalcitonin test was added to the pathway to better assist in guiding antibiotic therapy and/or resolving any uncertainty in regard to bacterial infection. This allows for the provider to guide earlier antibiotic discontinuation. Antibiotic de-escalation was previously recognized as an area for quality improvement.
- During drill downs, if areas of opportunity were identified, letters were drafted and sent to providers in order to suggest alternatives for improvement.
To sustain ongoing use of the order set and promote awareness of its benefits, key members of the team participated in a campus road show. Those campuses were prioritized in in-person lecture of the order set based on their pneumonia order set utilization rate.
Improving Patient Outcomes
The following measures were established that would be monitored throughout the duration of the project phase in addition to their baseline measurements:
Process Measures were monitored below to determine how these measures would be integrated into the electronic pneumonia guideline (order set):
- Urine/Legionella - frequency of orders and necessity to have these pre-checked on then pneumonia guideline, this would influence the clinical treatment plan of the patient by having these micro tests ordered and resulted.
- Sputum culture - rate of sputum cultures ordered and the necessity to have this pre-checked on pneumonia guideline.
- Oral care - frequency of this being ordered for nursing to complete and how often it is being completed. There was no established process for completing oral care across the network. Studies demonstrated that improved oral care reduced the risk of aspiration and hospital-acquired pneumonia.
- Order set utilization for pneumonia - the utilization rate across the network was 46%. Literature supported that leveraging order sets to drive clinical practice resulted in improved outcomes. After taking a general poll among multiple specialty providers, we learned that the pneumonia order sets were not easy to use and often lacked the treatment recommendations outlined by the IDSA.
The process measures discussed earlier were monitored using an Epic workbench report that was created for the process measures listed above. This workbench report was monitored weekly and performance was reported out monthly at pneumonia PI. The outcome measures were monitored monthly using the Network Pneumonia scorecard managed by clinical analytics and reviewed monthly at pneumonia PI. Statistical analysis would also be used to determining the significance of the outcomes (Figures 1 & 2). Additionally, a system list was created in Epic to monitor pneumonia patients daily for treatment opportunities, and real-time feedback was provided. As mentioned earlier, order set utilization was initially not an available report. In working with Epic analytics, a report was created to track and trend utilization over a period of time which would signify adherence to the pneumonia guideline (Figure 4).
Figure 2 & 3- Outcome measure comparison for those patients who used the order set versus those who did not use the order set (CY 2018 and 2019 performance)
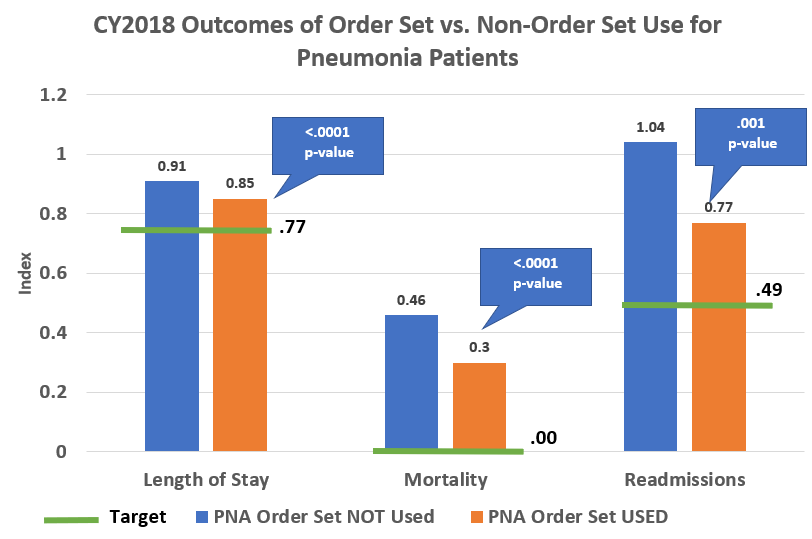
Source: St. Luke’s University Health Network

Source: St. Luke’s University Health Network
Figure 4: Tableau Order Set Utilization
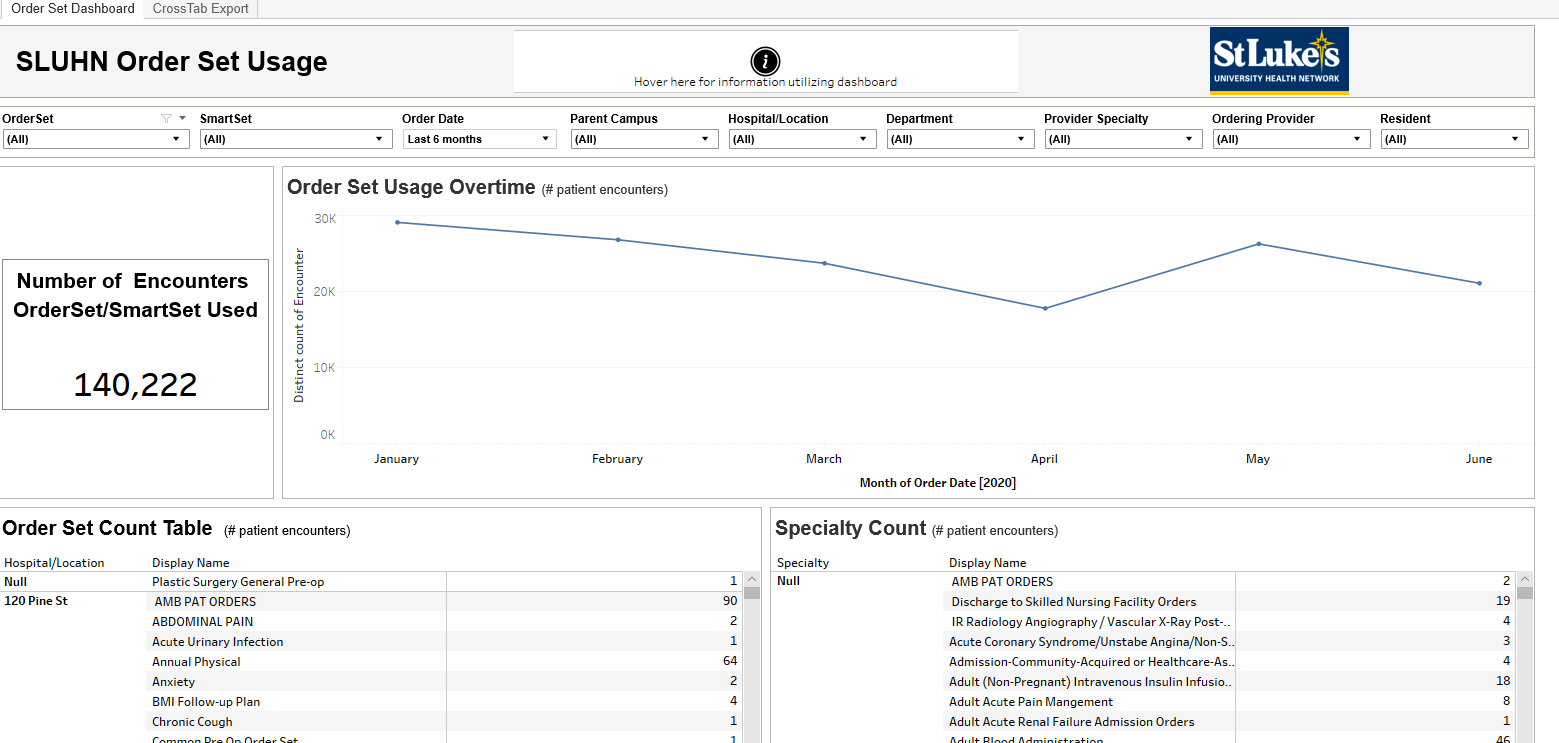
Source: St. Luke’s University Health Network
Accountability and Driving Resilient Care Redesign
- When looking at above figures 2 &3 noted is a 35% reduction (statistically significant) in mortality for those who used the order set when compared to those who did not use the order set. A 26% reduction (statistically significant) in readmissions for those who used the order set was noted.
- It was also noted that a 60% increase in oral care documentation, occurred after education and product was made available.
- There was an overall network cost avoidance of > $3,370,561.
- Buy-in from leadership as well as multidisciplinary engagement from practicing teams within the network was a key success factor.
- Additionally, ongoing transparency of data with the ability to constantly share information and feedback on progress was important to correct practice in real time and continually monitor progress.
- It was important to engage service line leadership to see the value in utilizing order sets for improved outcomes and continued to educate about the best practices in the clinical management of pneumonia.
- Sustaining and improving on outcomes in FY’19 was priority. The ability to develop improved data collection was pertinent.
- The ability to run reports daily allowed for quicker ability to intervene or advise.
- Daily system reports are able to be reviewed.
- A specific folder of all actively diagnosed pneumonia patients within the network can be accessed at any time, for periodic spot checks and chart review.
- The ability to review order set utilization at any time (reports can be run daily).
The views and opinions expressed in this content or by commenters are those of the author and do not necessarily reflect the official policy or position of HIMSS or its affiliates.
HIMSS Davies Awards
The HIMSS Davies Award recognizes the thoughtful application of health information and technology to substantially improve clinical care delivery, patient outcomes and population health.



