Executive Summary
The percentage of sepsis patient cases meeting bundle requirements was below benchmark and there was opportunity to improve both mortality and length of stay (LOS).
Key Stakeholders
Medical Staff, nursing, performance improvement, virtual sepsis unit (VSU), healthcare informatics, laboratory personnel, pharmacy and patients.
People, Process and Technology
- Interdisciplinary Committee, established December 2017
- Assign patient champions
- Ongoing Physician Education (Team Health EDP group onboard)
- VSU/eICU (PCU/ICU and Med-Surg Units) April 2017; January 2018
- Sepsis Handoff Tool – May 2019
- Dashboards
- Sepsis Bundles
- Device integration
- Bedside specimen collection and scanning
- Clinical decision support (CDS)–Alerts
- Care team communication
Outcome
The sepsis patient mortality rate decreased from as high as 1.91 in Q1 2017 to as low as 0.45 in 2019. Cases meeting the bundle compliance increased from as low as 52% in Jan 2018 to as high as 88% in August 2019. LOS also decreased from a high of 6.83 days on average in January of 2017 to as low as 3.88 days on average in August of 2019.
Lesson Learned
- Teamwork and collaboration were instrumental in the success of bundle build and increasing bundle compliance. Accountability and the ability to measure outcomes and compliance are critical
- Assign a patient champion who is an expert in sepsis management
- Utilization of a VSU such as an eICU provides another layer of surveillance.
- CDS, alerts, dashboards and direct communication with the care teams are part of the direct communication in place to improve care.
Define the Clinical Problem and Pre-Implementation Performance
Local Problem
Our goal was to reduce clinical variation in the care of sepsis patients at Homestead Hospital and throughout the system at Baptist Health South Florida (BHSF). We engaged the care team in improving processes related to the treatment of patients presenting to respective Emergency Departments (ED), via direct admission, or who become septic during their stay.
Background
Sepsis affects over 26 million people worldwide every year, and the organization treats over 3,000 patients annually with sepsis, severe sepsis or septic shock. Sepsis is the body’s response to an infection that has become overwhelming and can lead to tissue damage, organ failure, amputations and death. Mortality increases 8% for every hour that treatment is delayed and as many as 80% of sepsis deaths could have been prevented with rapid diagnosis and treatment. Sepsis patients have the largest cost of hospitalizations in the United States consuming more than $24 billion dollars each year. Sepsis patients also have almost double the average cost per stay at around $18,400 per admission.
Previous work to improve bundle compliance was achieved through the BHSF Accelerated Change Team (ACT), which developed system wide order sets. The reflex lactate was also implemented through the BHSF ACT enabling lab to automatically order a timed lactate to achieve follow-up lactate compliance.
Homestead Hospital has a robust sepsis patient committee that meets monthly, reviewing outcome measures and providing education, mock codes, as well as reviewing cases month to month. The organization partnered with Navigant on the T2020 initiative which includes redesigning care for select DRGs. Navigant and the organization decided upon a structure of a Sepsis Steering Committee as well as two design groups: An ED team and an inpatient and ICU team. These teams collaborated on creating clinical specification to ensure sepsis patients got the same care every patient, every time. BHSF facilities such as Homestead Hospital had varied levels of success in completing the Centers for Medicare and Medicaid Services (CMS) 3-hour and 6-hour bundles for patients identified as septic. The inconsistency of implementing the two bundles in a timely manner led to significant LOS and improved mortality opportunities. Earlier identification and implementation of the interventions described in the bundles led to better outcomes for sepsis patients and a decrease in the LOS.
Outcome
The mortality rate decreased from as high as 1.91 in Q1 2017 to as low as 0.45 in 2019. Sepsis patient cases meeting bundle compliance increased from as low as 52% in Jan 2018 to as high as 88% in August 2019. LOS also decreased from a high of 6.83 days on average in January of 2017 to as low as 3.88 days on average in August of 2019.
All patients >18 years of age are screened for sepsis, the numerator is the total count of patients treated in compliance with the bundle and the denominator includes all patients with the MS-DRG of sepsis (positive screen). Mortality rates are based on severity adjusted benchmarks and LOS is based on the average LOS against the benchmark of CMS and Premier.
Targeted performance
To meet and/or exceed the benchmark.
Benchmark data
BHSF benchmarks sepsis patient data against CMS, the Acute Physiology And Chronic Health Evaluation (APACHE) IV severity of disease classification system (ICU/PCU), Premier, and internal goals.
Technology initiatives
Electronic health record (EHR) data, CDS such as the St. Johns Sepsis Alert, clinical dashboards, Ascom phones for communication, the eICU for virtual care management, bedside specimen collection scanning, device integration for clinical data and bundle management via PowerPlans™.
People and Process
The evidence-based clinical care (EBCC) committee oversees the organizational structure for process waves which identify areas for improvement. The VSU is a component that enhances people, process and technology. The sepsis patient champions help to optimize infection management and emphasize the importance of early recognition and timely treatment, they also facilitate sepsis patient care and optimize patient outcomes. Ongoing physician and team education are available via lunch and learns with classroom time, elbow to elbow support, web-based learning, online formats on the EBCC website via the intranet and on the Baptist Health South website which is available in the public domain. The continuing education is a vital component to the hospital-wide code rescue response team.
Design and Implementation Model Practices and Governance
Baptist Health South Florida’s EBCC initiative is a strategic system-wide standardization effort to reduce variation and unnecessary costs while focusing on evidence-based, quality care. The process is driven by key stakeholders and is supported by real-time, statistically supported benchmarked data. The charter was signed in 2016 and provides the foundation for a methodical approach to improve patient outcomes (Figure 1).
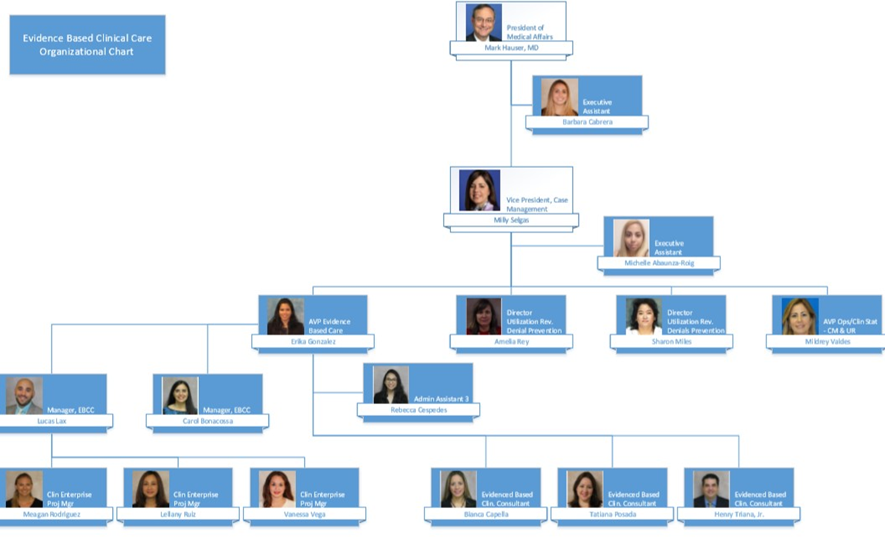
Source: Baptist Health South Florida
The methodology begins with a call to action to for an evidenced based care assessment of current and future state, design plan, team approval, development of an implementation plan, measurement and sustainment plans (Figure 2).
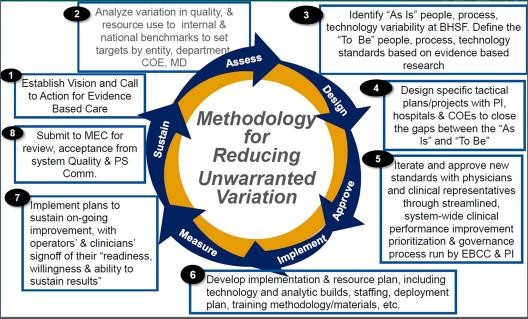
Source: Baptist Health South Florida
Each specific project is supported by a sub-group who are experts in on the focus topic. The Service Line Collaborative includes:
- Cardiac and Vascular
- Critical Care
- Emergency Department
- Gastrointestinal
- Hematology
- Infectious Disease
- Neonatology
- Nephrology
- Neuroscience
- OB/GYN
- Oncology
- Orthopedics
- Pharmacy
- Pulmonary
- Sepsis
- Surgery/PEI/ERAS/NSQIP
Navigant and BHSF decided upon a structure for a Sepsis Steering Committee to reduce variation in the management of sepsis to improve the sepsis patient mortality rate.
Education was completed via lunch and learns with classroom time, online formats on the EBCC website via the intranet and on the organization’s website which is available in the public domain.
PowerPlan™ education is a consistent part of physician education and CME education is available with every MS-DRG or pathway as it rolls out. The pilot for the sepsis patient go-live began in February 2017 and the hospital wide go-live was April 2017. The iterations over time have continued based on new benchmarks and evidence as it becomes available.
Technologies include: the physiologic data within the EHR, device integration, CDS, bedside specimen collection, sepsis algorithm, support from the eICU/VSU, dashboards and PowerPlans™ for the care bundle.
Clinical Transformation enabled through Information and Technology
To reduce clinical variation in the care of sepsis patients throughout the health system at BHSF, we engaged the care teams to improve processes related to the treatment of patients presenting to respective EDs, via direct admission, or who become septic during their stay. The workflows are geared to meet the care requirements as outlined by the industry in evidenced based research such as CMS and the Society of Critical Care Medicine’s Surviving Sepsis Campaign (Figure 3). While the overarching goal is the same throughout the venues of care, the workflows are created to meet clinical specification to ensure sepsis patients get the same care—every patient, every time. The utilization of the bundle is the foundation for minimizing the variation in care, and the people, process and technology as overseen by the EBCC committee provides the balance to drive action.
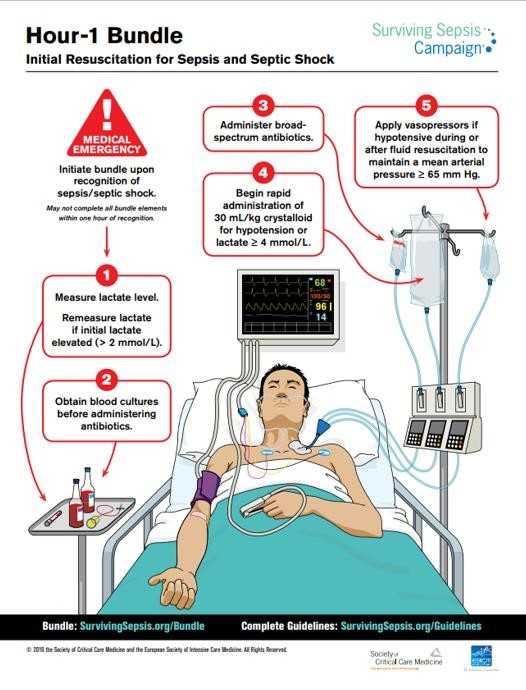
Source: Baptist Health South Florida
The workflows for the ED begin at triage and lead to the engagement of the VSU (Figure 4). The VSU is “air traffic control” for compliance and workflows are also designed for the ICU/PCU and med/surg areas (Figures 5 and 6). The VSU is operated out of the eICU and the virtual team streamlines the workflows to improve compliance to CMS guidelines, improving outcomes and reducing reimbursement penalties.
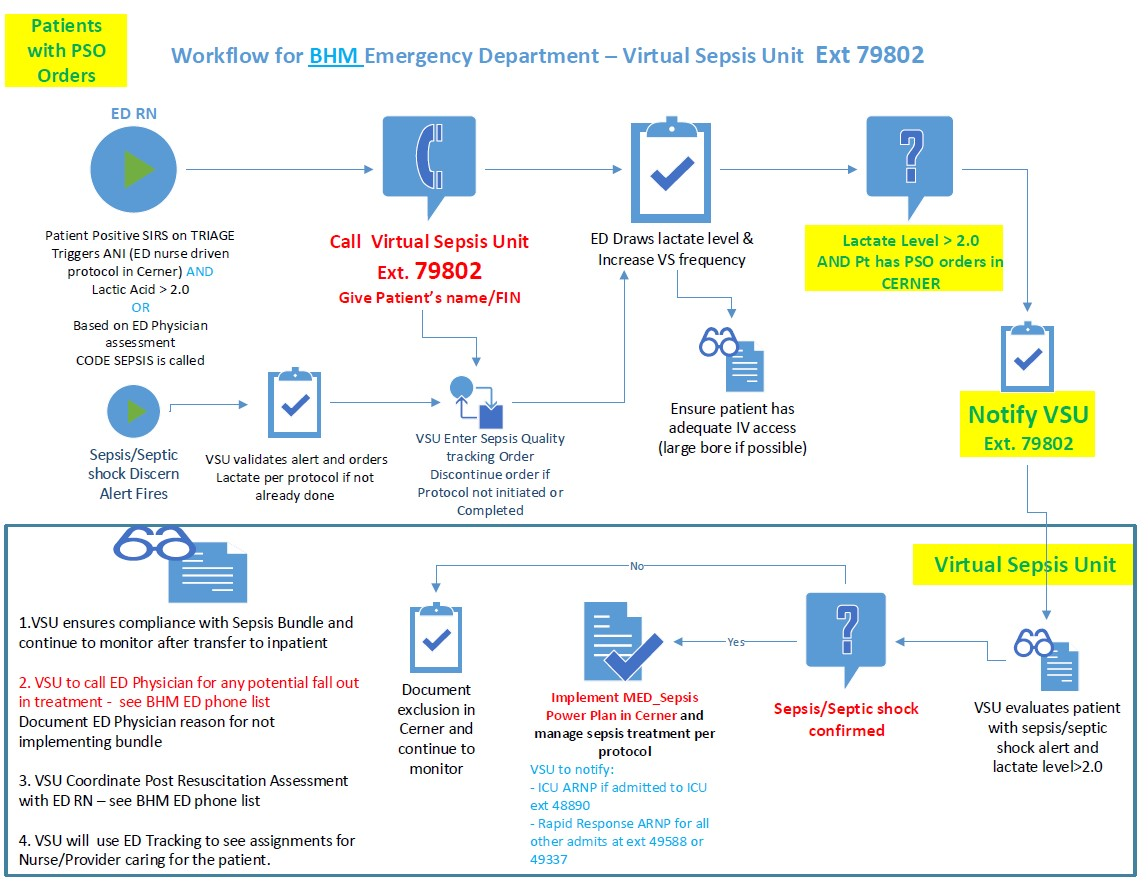
Source: Baptist Health South Florida
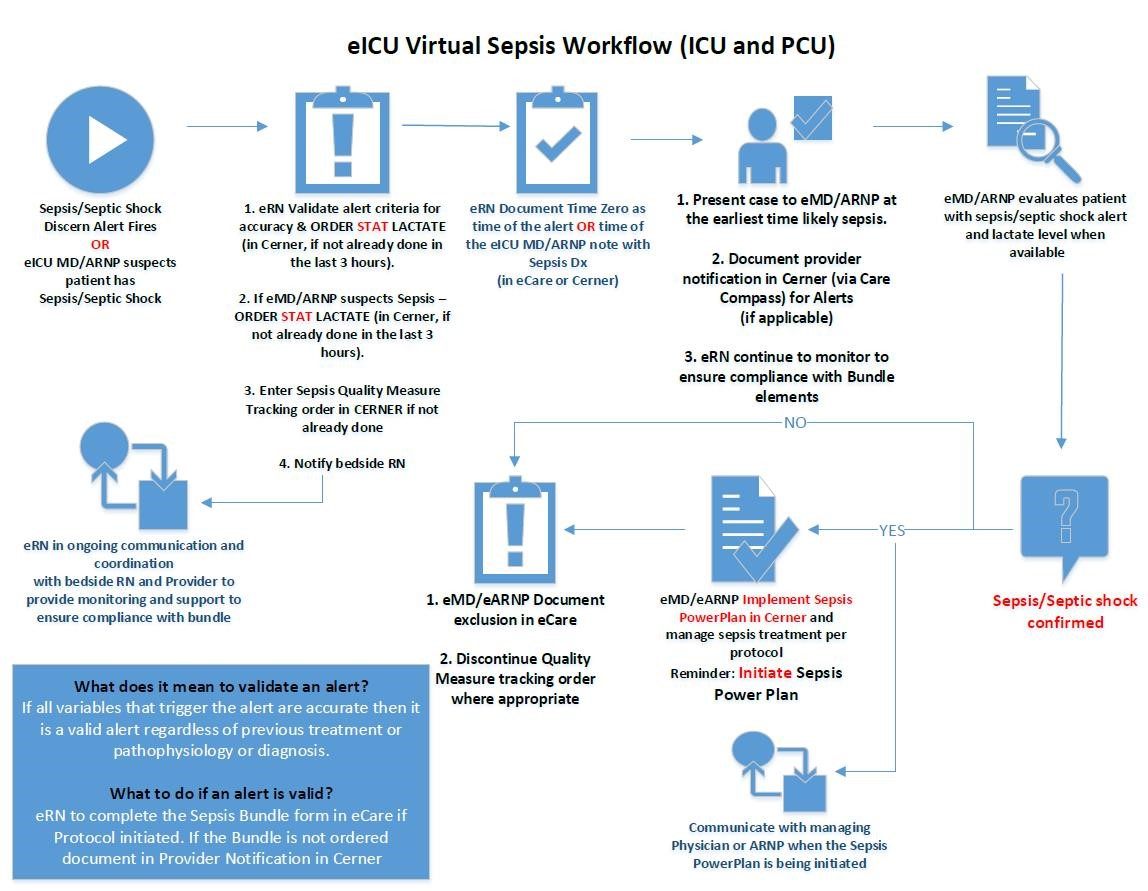
Source: Baptist Health South Florida
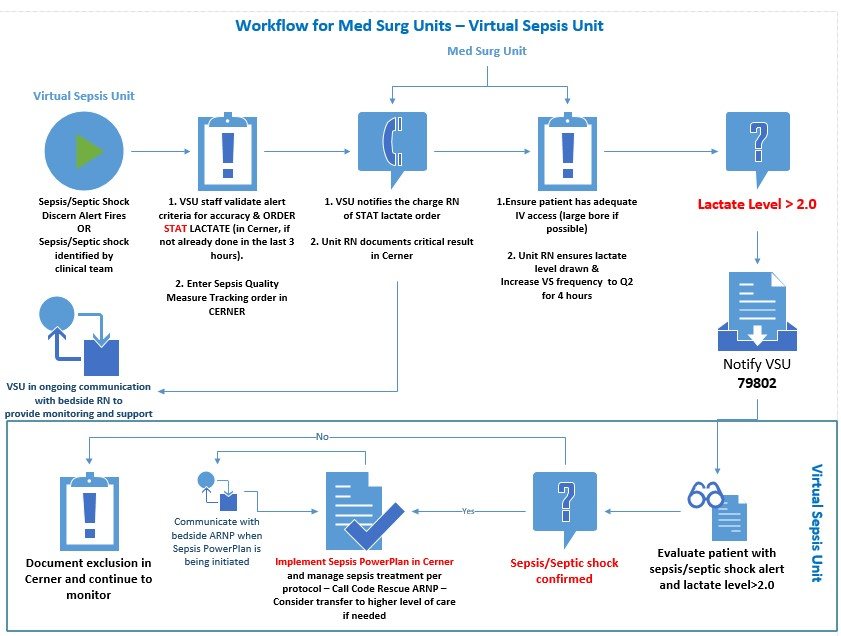
Source: Baptist Health South Florida
The algorithm that drives the alert is embedded into the EHR (Figure 7). The EHR supplies the clinical data required for the alert by integrating technologies such as vital sign devices, bedside specimen collection and scanning and lab values. Dashboards are available in the VSU, ED and nursing units to enhance access to the alerts, as well as alerting within the EHR.
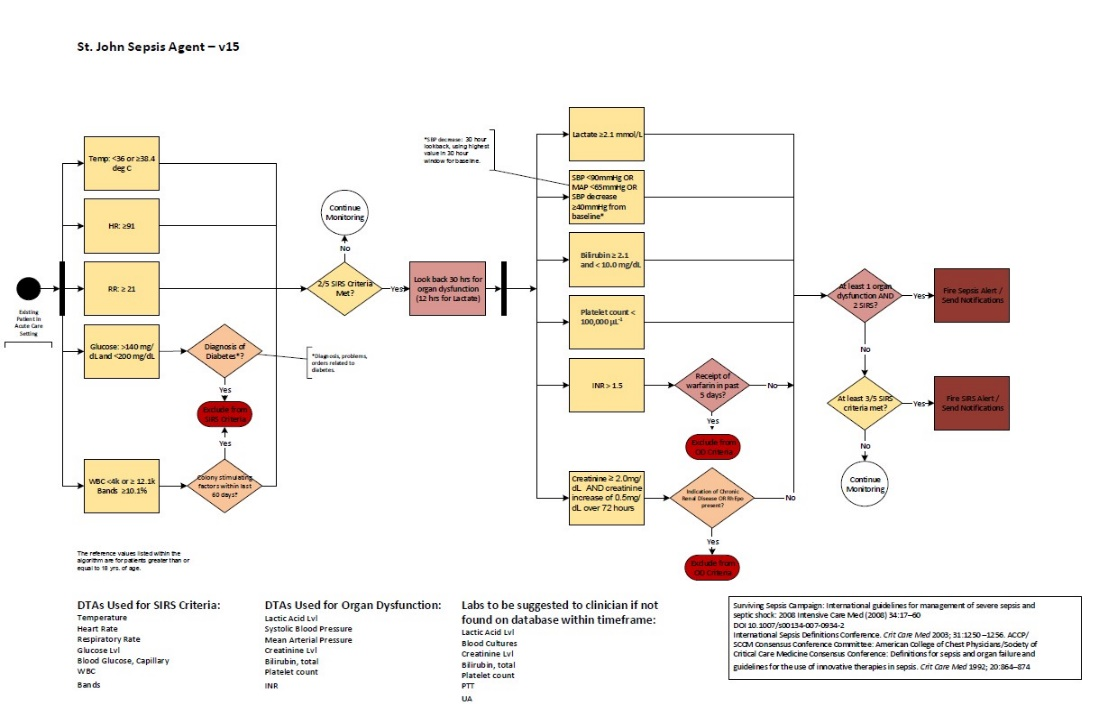
Source: Baptist Health South Florida
Documentation of care takes place in the EHR and the CDS for the algorithm generates the alert (Figure 8).
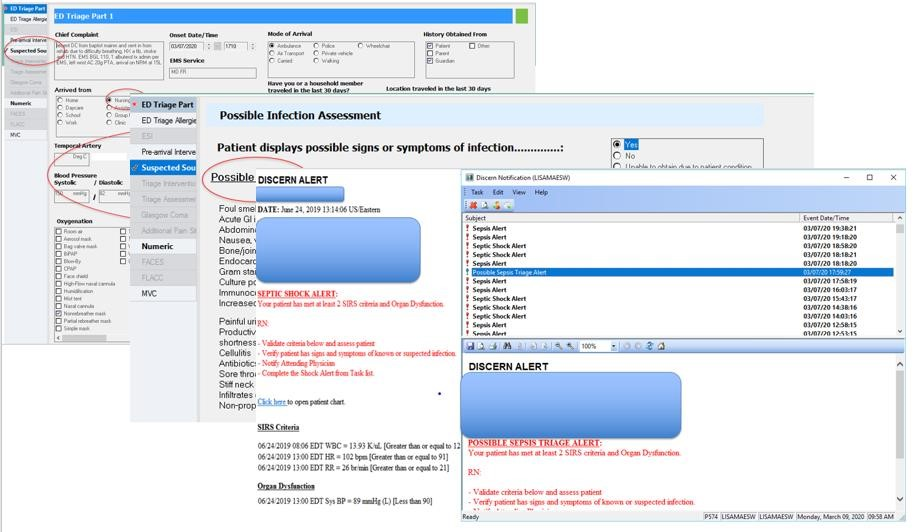
Source: Baptist Health South Florida
Managing the alert volume to prevent alert fatigue is a key responsibility of the VSU. The VSU reduces the number of non-actionable alerts going to physicians and nurses. Fewer alerts help to improve the specificity of the alert and provides clinical validation. (Figure 9).
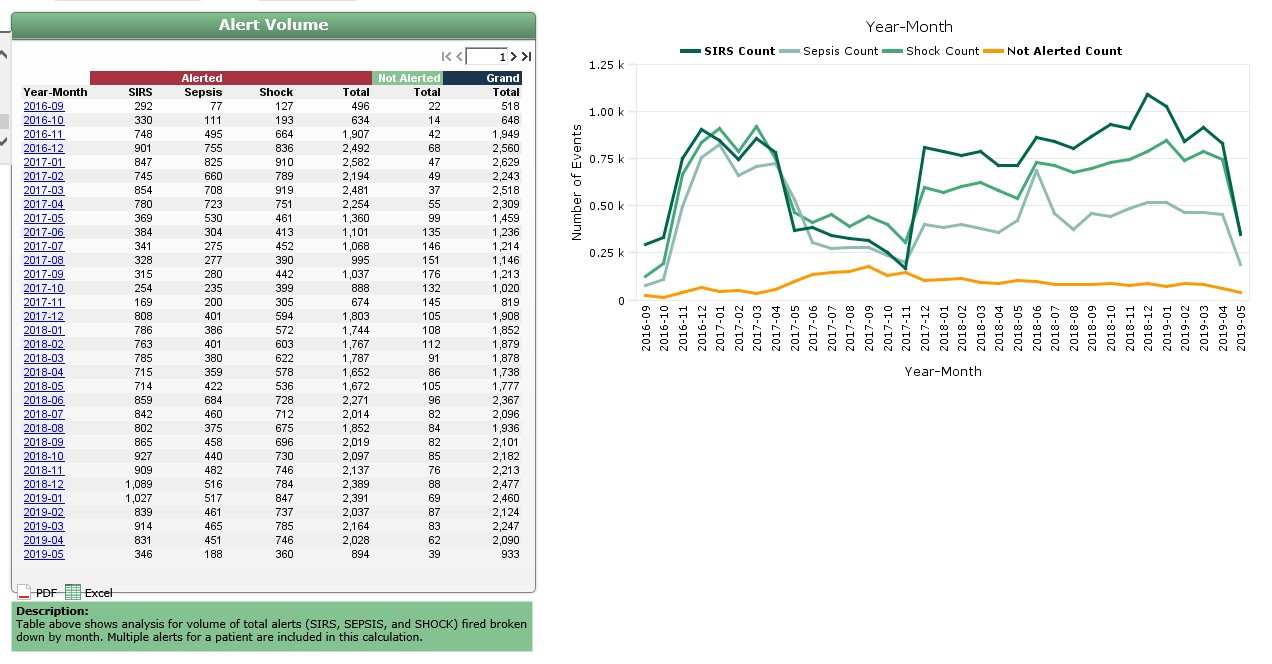
Source: Baptist Health South Florida
In 2019, new guidelines were released for the recommendation of lactate measures and these recommendations were built into the bundle and the workflows (Figure 10).
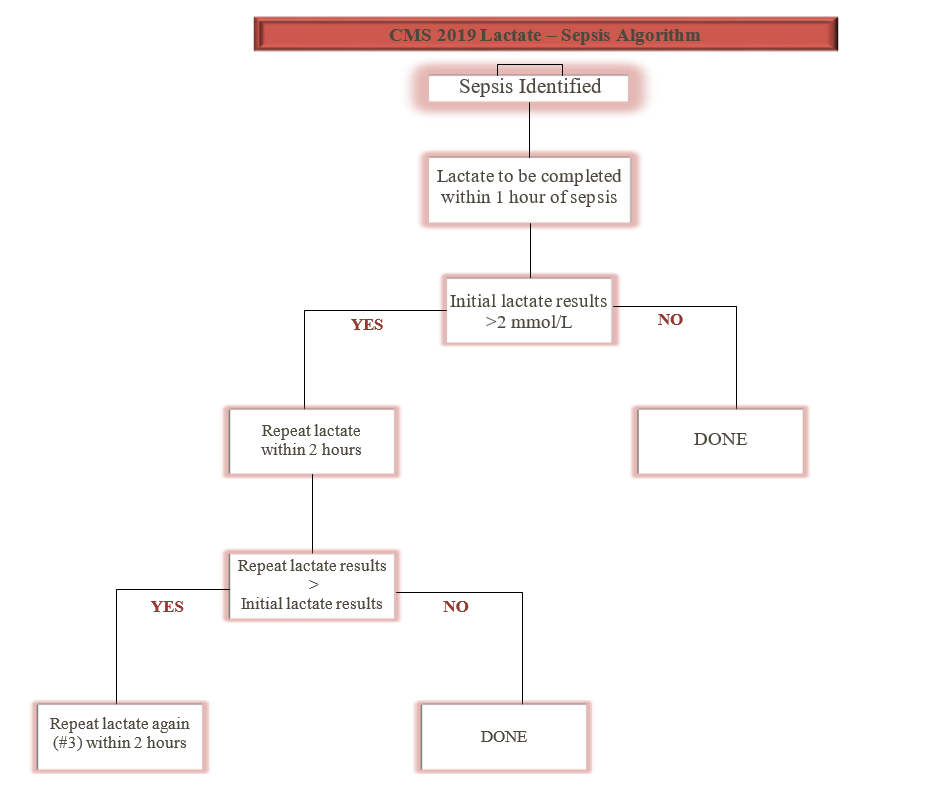
Source: Baptist Health South Florida
Examples of documentation for the bundle includes suspected sepsis patient and a quick bundle (Figure 9). Education for all care is available in the electronic version of ‘what I need to know’ (eWINK), a BHSF online education tool in the public domain which also offers CMEs/CEUs. Education for staff also includes lunch and learns with classroom time, elbow to elbow support and online formats on the EBCC website via the intranet. PowerPlan™ education is a consistent part of physician education and WINK collateral, CME education is available with every MS-DRG or pathway as it rolls out (Figure 11).
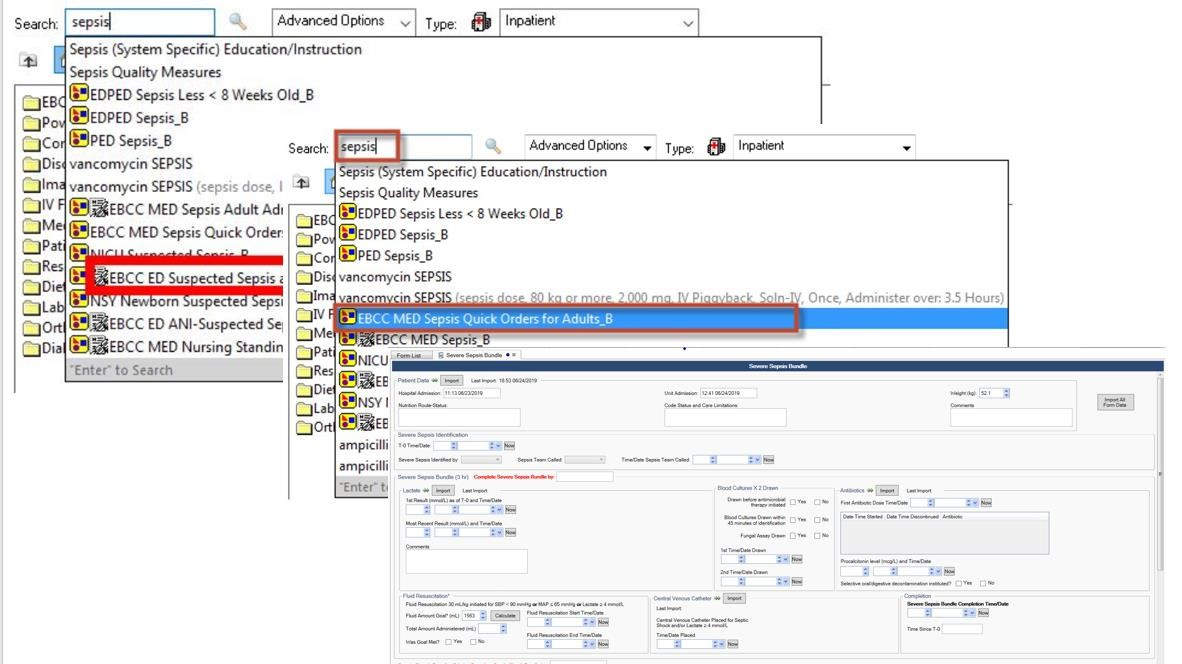
Source: Baptist Health South Florida
Using existing infrastructure of the eICU, virtual sepsis management was incorporated into exiting workflows. PowerPlans™ are used for bundle documentation, integration of clinical data within the EHR is supported by device integration and specimen collection and the EBCC drives pushing the current evidence to the point of care and keeps the educational material up to date.
Improving Adherence to the Standard of Care
All patients >18 years of age are screened for sepsis upon triage in the ED and all inpatients >18 years of age are monitored via CDS surveillance with the sepsis alert running within the EHR. The numerator is the total count of patients treated in compliance with the bundle and the denominator includes all patients with the MS-DRG of sepsis (positive screen). The organization transitioned to the current EHR in September of 2016 and implemented the bundle PowerPlans™ and sepsis initiative in 2017. Prior data indicated the facilities had varied levels of success in completing the bundles for patients identified as septic and the inconsistency led to opportunities to improve LOS and mortality rate.
Over time, at Homestead Hospital the compliance rate for the CMS 3-hour sepsis bundle increased from ~35% in 2015 to >90% in February 2020, with the data steward being CMS (Figure 12).
Homestead Hospital followed the standard process of change management and care redesign as outlined in the EBCC methodology. The EBCC is the governing body driving the utilization of evidence-based care focused on eliminating variation in care delivery.
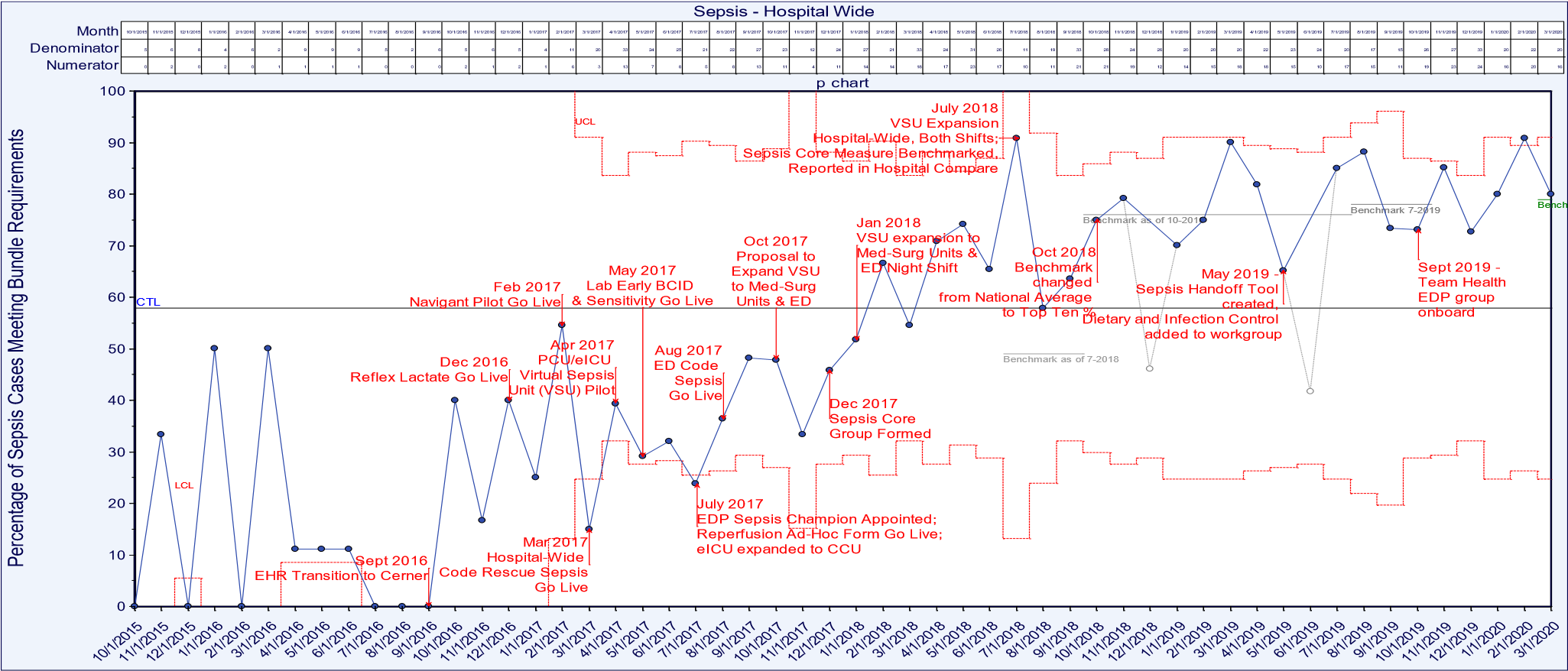
Source: Baptist Health South Florida
Improving Patient Outcomes
The sepsis severity adjusted mortality rate decreased from as high as 1.91 in Q1 2017 to as low as 0.45 in 2019 (Figure 13). Average LOS also decreased from a high of 6.83 days on average in January of 2017 to as low as 3.88 days on average in August of 2019 (Figure 14). The risk adjusted mortality and O:E ratio are generated from Premier data.
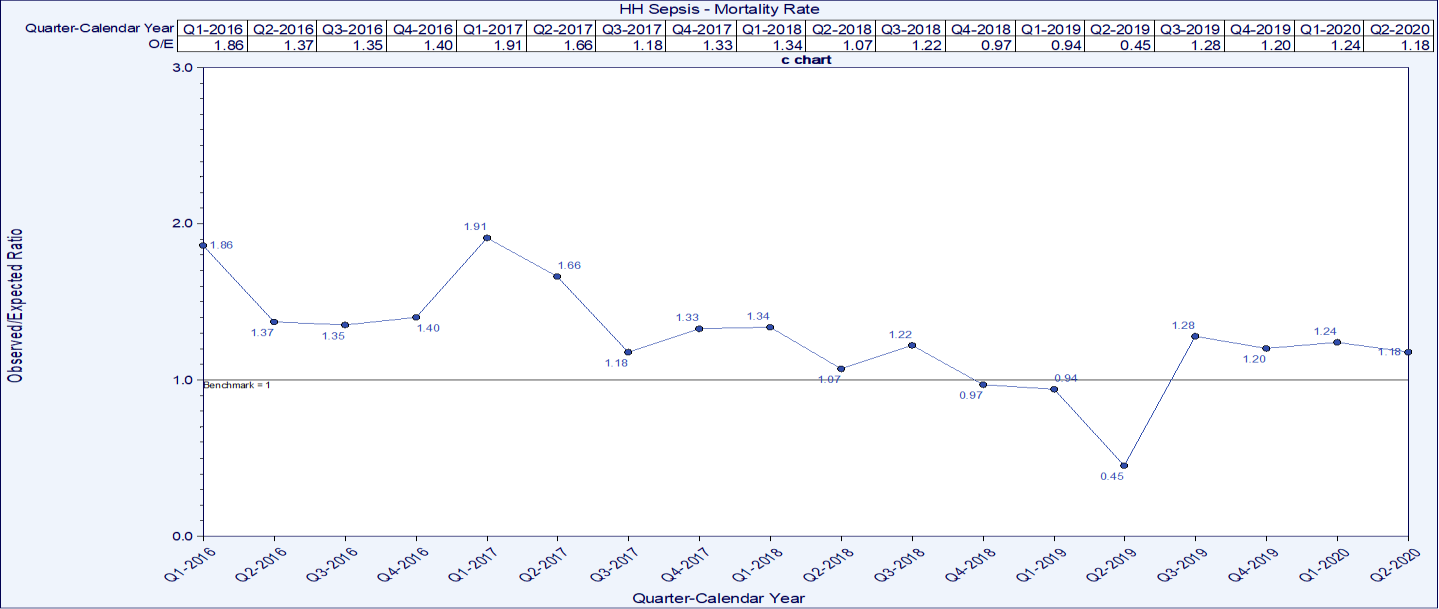
Source: Baptist Health South Florida

Source: Baptist Health South Florida
Accountability and Driving Resilient Care Redesign
BHSF and Homestead Hospital rely on a data driven and evidence based clinical care approach to guide the design and implementation of sepsis patient care bundles. The goals of the organization’s EBCC are to decrease variation across the clinical areas and provide predictable, data-driven high quality, affordable care. Having the tools to collect as close to real-time as possible compliance data and report on that data in near-real-time reflects the ability of the organization to target and successfully improve care delivery, and ultimately improve the clinical outcomes.
In near-real-time, the clinical team document the compliance of bundle utilization and the data is then accessible in their DivePort analytics dashboard (Figures 15 and 16). The dashboard is designed to provide statistical analysis, benchmark information and severity adjusted data with the capability to drill in multiple layers.
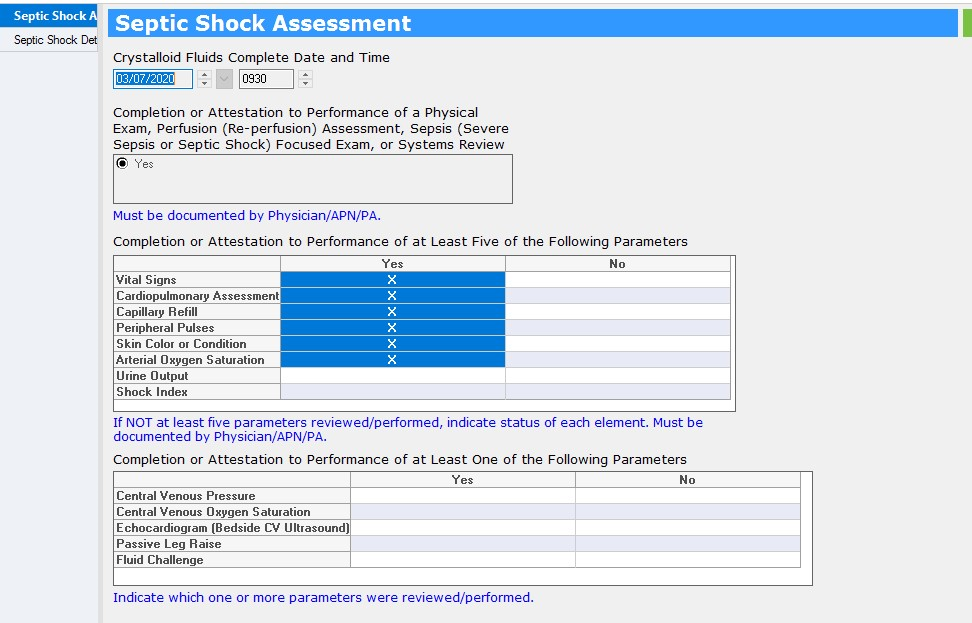
Source: Baptist Health South Florida
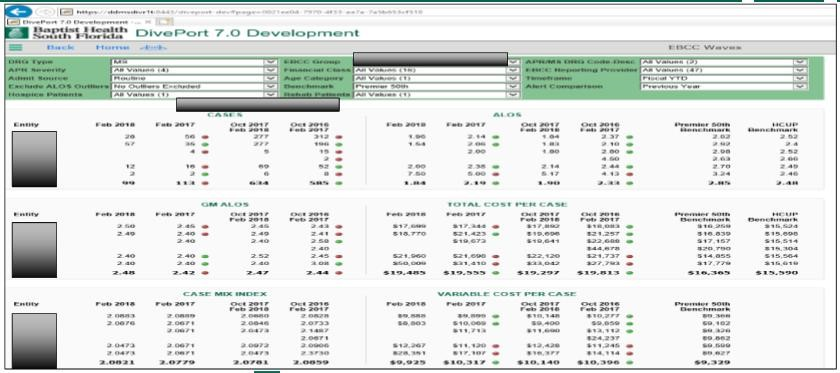
Source: Baptist Health South Florida
PowerPlans™ and bundle utilization is also available in DivePort, lending to the capability of measuring and reporting not only on the outcomes, but also to the compliance of the guidelines (Figure 17).
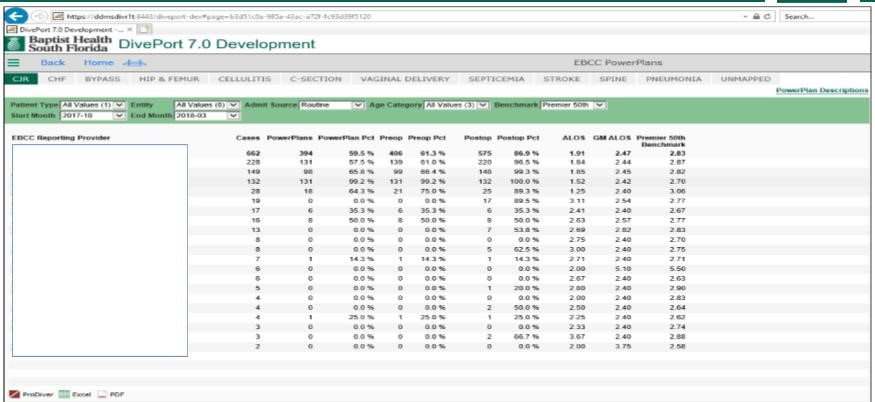
Source: Baptist Health South Florida
Using analytics to find variation
- APR-DRG Population Group is identified based on cost opportunity when compared to HCUP 40th percentile (Total Cost Per Case and ALOS).
- EBCC and Analytics Integrity Committee members review MS-DRG specific groupings that correspond with APR-DRG grouping.
- Premier benchmark levels of 50th and 75th percentile variable cost opportunities are used to further validate the data.
- MS-DRGs are recommended for EBCC team redesign based on variable cost opportunity, average LOS and volume.
- EBCC DivePort 7.0 Portal reporting is updated as DRGs waves are defined for tracking outcomes.
The rollout of the VSU is an example of using data to further refine the care redesign to complement the people, process and technology to enhance care delivery (Figure 18).
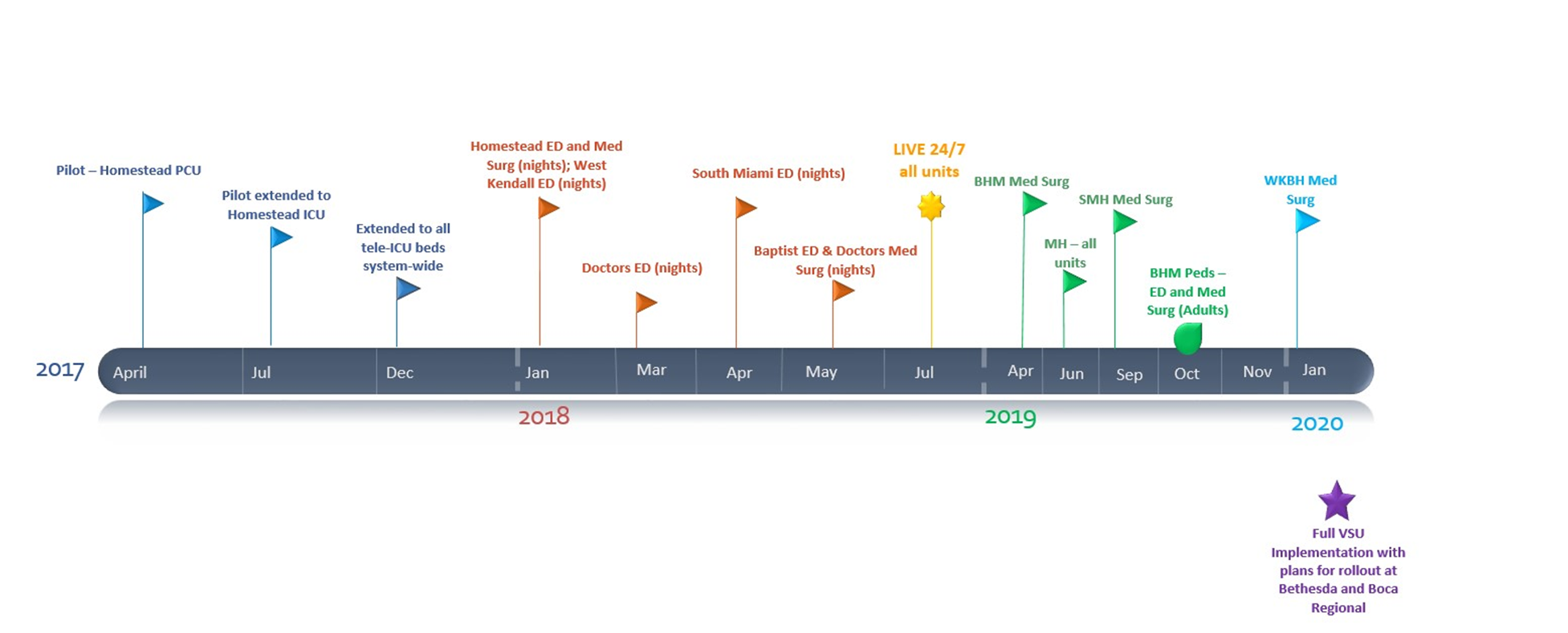
Source: Baptist Health South Florida
The views and opinions expressed in this content or by commenters are those of the author and do not necessarily reflect the official policy or position of HIMSS or its affiliates.
HIMSS Davies Awards
The HIMSS Davies Award showcases the thoughtful application of health information and technology to substantially improve clinical care delivery, patient outcomes and population health.



